
Key Takeaways
AI becomes essential infrastructure: Clinical decision support systems now achieve diagnostic accuracy comparable to specialists, while ambient documentation reduces physician burnout from 50.6% to 29.4%.
Revenue cycle automation delivers measurable ROI: Organizations implementing comprehensive RCM solutions report 30-40% fewer billing errors and denial rates dropping from 14% to below 5%.
Cybersecurity threats demand zero-trust architecture: Healthcare data breaches now cost $10.93 million on average, with ransomware incidents increasing 42% and requiring immediate defensive action.
Cloud-native interoperability becomes standard: 70% of healthcare organizations have migrated to cloud systems, while FHIR APIs enable seamless data exchange mandated by the 21st Century Cures Act.
Edge computing transforms point-of-care delivery: By 2026, 75% of medical data will be generated at the edge, providing real-time insights and maintaining operations during network outages.
Healthcare IT is undergoing a fundamental transformation as we approach 2026, with AI commanding 54% of venture capital investments and physician adoption surging from 38% to 66% in just one year. The future looks different with cloud-native data platforms taking over traditional departmental IT models, and ambient clinical documentation has become standard practice rather than just an innovation.
Healthcare faces some tough challenges ahead. Experts predict uninsured rates might double by 2026, and rural health workforce shortages could rise by 10%. Healthcare organizations should prepare for these changes before the next HIMSS conference. This preparation will help them stay competitive and provide the best patient care.
This piece explores everything in healthcare IT that will shape 2026 -- from AI and machine learning breakthroughs to the interoperability solutions that will define healthcare's future.
AI and Machine Learning Taking Center Stage in Healthcare IT

AI and digital health tools have gained massive acceptance among physicians. Their adoption rates jumped from 38% to 66% in the last year. This surge shows how AI has become a core strategic component rather than just an add-on technology.
Clinical Decision Support Systems Maturation
Clinical decision support systems (CDSS) have come a long way since their debut in the 1970s. Modern AI-powered CDSS can now process huge datasets, spot complex patterns, and customize recommendations based on patient needs. These systems have shown amazing results -- some AI tools match trained dermatologists in accuracy when they classify certain skin cancers. These technologies also excel at spotting unusual patterns and predicting clinical outcomes, especially for conditions like heart failure.
Ambient Clinical Documentation Becomes Standard
Ambient clinical documentation has moved from experimental tech to everyday practice. Mass General Brigham saw clinician burnout drop from 50.6% to 29.4% after they started using ambient AI documentation. Emory Healthcare's numbers tell a similar story -- their clinicians who felt documentation practices helped their well-being jumped from 1.6% to 32.3%. A UChicago Medicine survey revealed that 90% of clinicians could give patients their full attention after implementation, up from 49% before.
AI Governance and Regulatory Frameworks
AI has become deeply woven into clinical infrastructure, making governance frameworks crucial. Last year, all 50 states proposed AI legislation, and nearly 40 states adopted about 100 measures. Health systems need organization-wide frameworks that ensure responsible AI use, including proper training and appropriate guardrails to stay compliant.
ROI Measurement and Value Demonstration
AI proves its worth beyond just making operations better. Predictive sepsis detection cuts ICU stays, saving $1,500 to $3,000 per case -- adding up to $1-2 million yearly for a typical 100-bed hospital. AI tools for heart failure management can save between $8,000 and $12,000 each time they prevent a readmission.
Meet RSA Tech at HIMSS 2026
We'll be at HIMSS 2026 in Las Vegas from March 9-12, and we'd love to meet you. Whether you're a CIO working on your AI strategy, a CTO building governance frameworks, or a clinical informatics leader exploring AI solutions -- let's talk about how AI-first managed services can help you move from pilot to production faster.
Revenue Cycle Management Integration Into Clinical Workflows
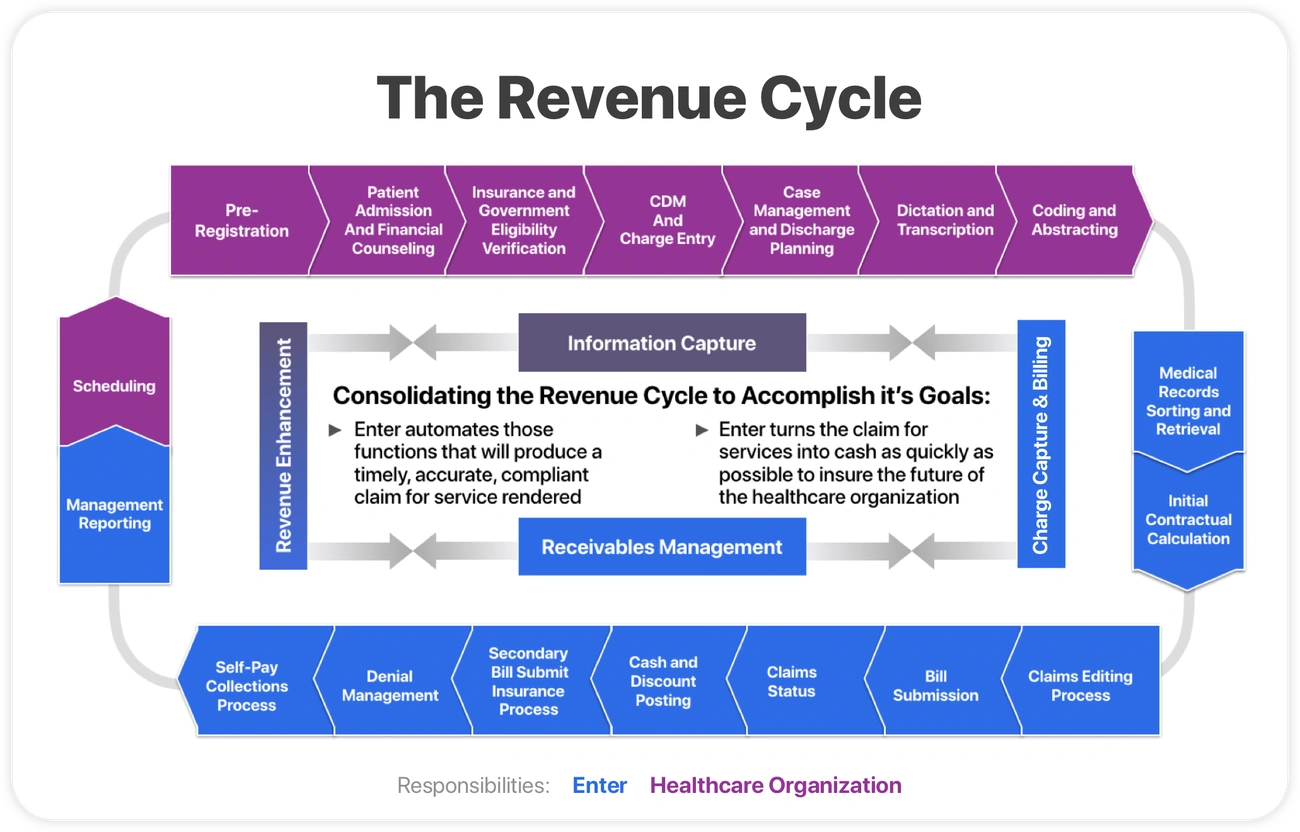
Healthcare's revenue cycle management operations face tough integration challenges today. One-third of authorization tasks still need manual handling through phone, fax, or email. Only 31% use fully electronic methods. Other healthcare technologies have advanced, yet RCM processes trail behind claims submissions (98% electronic) and eligibility verification (94% electronic).
Front-End RCM Automation Tools
Modern platforms establish the foundations of successful revenue cycle management before patients arrive. These systems connect scheduling, registration, and patient financial counseling. Industry data shows that clinics with connected systems process payments 20-25% faster and reduce billing errors by 30-40%. This allows organizations to shift their core team from paperwork to patient care.
Prior Authorization Process Optimization
Authorization inefficiencies create major bottlenecks. About 95% of healthcare organizations report patient care delays or denials because of prior authorization requirements. The Centers for Medicare & Medicaid Services Final Rule requires FHIR-based electronic prior authorization systems with strict turnaround times -- 7 days for standard requests and 72 hours for urgent ones. Organizations that use electronic prior authorization solutions save an average of 11 minutes per transaction, which could help the industry reduce costs by $317 million.
Real-Time Eligibility Verification
Instant eligibility verification has become essential, especially with rising denials. This technology lets providers instantly validate active coverage, copays, deductibles, and service-level benefits during scheduling or check-in. Healthcare providers that use automated verification solutions see denial rates drop from 14% to below 5%. They also submit claims 32% faster and receive payments in 25 days instead of 42, leading to annual cost reductions over $250,000 in some cases.
Coding and Documentation Efficiency Gains
Clinical documentation shapes revenue cycle success. Physician-entered coding has been common until now, resulting in higher denial rates and revenue leakage. AI-powered coding automation helps solve this challenge -- studies show pediatric coding denial rates decreased from 34% to 8%, while primary care denials dropped from 26% to 9%. Healthcare organizations can now automatically map clinical terminology to accurate secondary codes, preventing underpayment without adding to the documentation workload.
Cybersecurity Resilience and Data Protection Strategies
Cybersecurity attacks in healthcare have reached alarming levels. Ransomware incidents jumped 42% in 2022, and healthcare data breaches now cost around $10.93 million -- 8% more than the previous year.
Zero-Trust Architecture Implementation
Zero Trust Architecture works on a simple rule -- trust no one by default. Healthcare organizations that use this approach need to track all network assets, verify identities continuously using multi-factor authentication, segment access based on job roles, monitor activity patterns with behavioral analytics, and automate responses to quarantine compromised devices.
Ransomware Defense Mechanisms
Hospitals deal with targeted attacks that put patient care at risk. The Health-ISAC 2025 report shows 458 ransomware attacks happened in 2024. Good defense needs clear plans about when to disconnect systems to stop ransomware from spreading. Organizations should create backup snapshots that can't be changed and practice responding to simulated attacks regularly. A solid communication plan helps keep everyone informed during an attack.
Third-Party Risk Management Protocols
Third-party vendors caused 74% of healthcare's cybersecurity problems in 2023. Healthcare organizations need their top leaders to support vendor risk reviews. They should build backup systems for vital operations, test their emergency plans often, and write clear steps for recovery.
HIPAA and State Privacy Compliance Updates
HHS suggested big changes to HIPAA Security Rules on December 27, 2024. These updates came after seeing large breaches rise by 102% between 2018-2023. Healthcare organizations must update their Privacy Notices by February 16, 2026. The new rules pay special attention to protecting substance use disorder information.
Interoperability and Cloud Infrastructure Modernization
Healthcare organizations need better data exchange systems to support their evolving clinical and technical needs. Next-generation care delivery models will rely on interoperability as their foundation in 2026. Better data flow will lead to improved outcomes and stronger patient involvement.
FHIR API Adoption Acceleration
Modern healthcare interoperability depends on API-based data exchange. These standardized protocols let EHRs, clinical systems, and digital health applications communicate securely. The 21st Century Cures Act now requires certified health IT systems to provide standardized API access to patient data by banning information blocking. FHIR APIs help healthcare technology advance faster because vendors and providers can build adaptable solutions without major system overhauls.
Cloud-Native EHR Migration Patterns
Most healthcare organizations (70%) switched to cloud-based systems by 2023. This change has boosted patient satisfaction scores and operational efficiency while reducing security risks from older systems. Cloud environments can adjust resources when patient volumes fluctuate, and cloud-based EHR systems also remove data silos and help departments and facilities share information better.
Edge Computing at Point of Care
Edge computing reshapes the healthcare landscape by processing data closer to its source and giving clinical teams real-time data analysis. By 2026, 75% of medical data will be generated at the edge. Edge devices process data onsite to keep operations running during network outages, provide ultra-low latency processing for critical procedures, and offer better security with fewer attack vectors for patient health information.
Data Exchange and HIE Evolution
Health Information Exchanges (HIEs) now move from manual and batch-based sharing toward real-time, event-driven systems. As Bob Watson, CEO of Health Gorilla, notes, "In the coming year, healthcare leaders will grow to see full interoperability as a critical foundation for truly patient-centered care." More organizations adopt API-first ecosystems that support quick innovation and vendor flexibility.
Legacy System Integration Challenges
Most healthcare providers (70%) still use legacy systems, which increases security risks, causes integration problems, and raises maintenance costs. Legacy systems rarely work with newer technologies, creating major integration obstacles. Despite these challenges, integrated clinical professional workstations can offer flexible ways to connect systems without complete rebuilding.
Conclusion
Healthcare IT is at a turning point as we look toward 2026. Technology adoption has picked up speed across many areas. AI and machine learning are no longer optional extras but have become essential tools. Physician adoption has jumped from 38% to 66%. Clinical documentation systems are now showing real benefits for providers -- reducing burnout rates and helping deliver better patient care.
RCM solutions are moving quickly toward complete automation. Healthcare organizations using detailed RCM solutions see big improvements -- they report 30-40% fewer billing errors and much lower denial rates. The growing number of ransomware attacks and data breaches means cybersecurity needs more attention than ever. Organizations now must have zero-trust architectures, reliable third-party risk management, and detailed incident response plans.
Cloud migration and better interoperability are changing how healthcare works. FHIR APIs have become essential for modern healthcare data sharing. Edge computing now brings live processing right to where patient care happens.
See you at HIMSS 2026. We hope to see you in Las Vegas, March 9-12. Our RSA Tech team would love to talk about how AI-first managed services can help speed up your progress from pilot to production. Whether you're a CIO working on AI strategy, a CTO building governance frameworks, or a clinical informatics leader looking at solutions -- we're here to help.